The Cycle of Insomnia and Its Recommended Treatment
Modern Life Makes More Insomnia Common
Almost everyone relates to that feeling of frustration at night when you can't sleep. But there is a big difference between a periodic bad night, and chronic insomnia. When you start spending <85% of the time you are in bed sleeping, this is called a night of transient insomnia. If this happens regularly, it is referred to as chronic insomnia. This can occur throughout the night, either at the beginning when trying to fall asleep, in the middle of the night, or if you wake up too early in the morning.
In 2008, the Institute of Medicine reported that 50-70 million people in the U.S. suffer from insomnia. Untreated insomnia is linked to Alzheimer's disease and almost every chronic illness. In addition, almost everyone can relate to being grumpy and less productive after a night of poor sleep. On average we are also sleeping a whole hour less than we did in the 50's, with some experts believing that the blue light and always on nature of technology is to blame. Among people who suffer from insomnia, the disorder has varying degrees of severity. There are three main classifications of insomnia: transient, acute, and chronic. Transient insomnia occurs for days to weeks. Acute insomnia lasts from three weeks to about six months, and chronic insomnia can last for years. Short-term stress or changes in the environment generally affect transient and acute insomnia, as opposed to chronic insomnia. Women are 1.4 times more likely to suffer from insomnia than men.
When you have chronic insomnia, a vicious cycle typically forms where stressors in your life feeds into being more alert and arousable at night, which causes sleep issues and bad associations between the bedroom and sleep and then increasingly more stress.
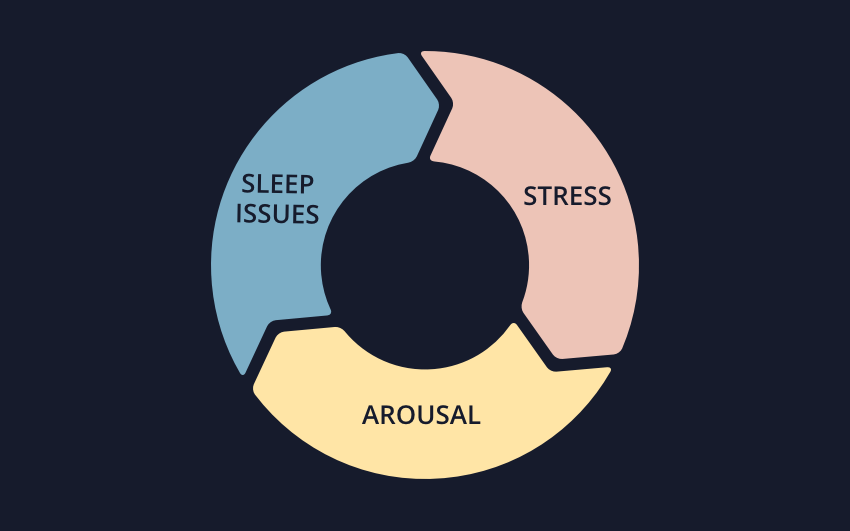
Insomnia is a vicious cycle...
While there are numerous drugs on the market that claim to relieve insomnia, the best way to combat the disorder is through behavioral treatment. The reason for this is because behavioral patterns often times are the causal culprit to this problem. Sleeping pills often come with the risk of dependency, and the clinical trials have shown them to typically reduce sleep onset by only about 10 minutes. What’s more is that sleep quality can be negatively impacted by these drugs. Cognitive behavioral therapies have no risk of dependency and can be more effective than medication. The problem is that to treat the number of insomniacs, each board certified sleep specialist would need to have around 8000 patients on their roster. SleepSpace has built technology to empower these clinicians to see more patients to finally address the problem of sleeplessness in America.
Cognitive-behavioral therapy
CBT includes the methods listed below and combines health practices and environmental factors that can promote or inhibit sleep. Factors like caffeine consumption, exposure to light, and room temperature can all affect sleep quality. If you believe you have insomnia, we recommend seeing a trained therapist in your area, which can be found here.

Stimulus Control Therapy
Stimulus control therapy means associating your bed and bedroom with sleep, and only with sleep. When we read, watch television, or do other non-sleeping activities in our bedroom, our brain associates this room with being awake and active. By re-associating the bed and bedroom with sleep, our brains then adjust to going to sleep and staying asleep when in bed. Stimulus control therapy can be very helpful in establishing a consistent sleep-wake schedule. The following steps are designed to create the association between sleep and your bed.
1. Go to bed only when you are sleepy
2. Get out of bed if you are unable to sleep
3. Use the bed/bedroom for sleep (and sex) only (no reading, watching television, talking on the phone, etc.)
4. Create a bedtime ritual, such as playing a certain sound or music when you go to bed or meditating
5. Go to sleep and wake up at the same times every day
Relaxation
When experiencing insomnia, it’s helpful to relax your body as well as your mind. Relaxation procedures aimed at relaxing both body and mind include progressive muscle relaxation, autogenic training, imagery training, meditation, and ambient sounds. Trying several of these techniques can help you find the ones that are best for you.
Paradoxical intention
Worrying too much about if you will experience insomnia or continuously checking how long you have been awake will impair your ability to fall asleep. It can be difficult to ignore your insomnia, but thinking about it will only further impair your ability to fall asleep. Reducing the amount to time that you think about or monitor your insomnia will help you to conquer it. When you find yourself worrying about if you’ll be able to fall asleep, try one of the relaxation methods described above such as focusing on breathing or relaxing your muscles. If you can’t sleep, be sure to get out of bed until you are sleepy again so that you don’t associate your bed with wakefulness.
What is an ideal environment to induce sleep?
Studies have shown that elevated body temperature can increase sleep onset, so you want a cool environment. Having a bedtime ritual is also important. Cognitive behavioral therapists will often say that the process of going to bed starts about a half hour before you actually get into bed. Meaning that it is useful to have bedtime rituals to tell your body when to relax. In the digital age when people are always on their devices, this can be particularly problematic. Leave the device in the other room and don’t be around too many bright lights. Sometimes a meditation ritual can help for those times that the mind is racing.
Cognitive Training
Another important component of addressing the issue of insomnia is cognitive training. What this means is addressing maladaptive thoughts that can form around your sleep issue, which then results in worse sleep. These thoughts typically involve those that produce more anxiety close to bedtime.
How do I address maladaptive thoughts?
We build the Dr. Snooze chatbot to help address some of these worrisome thinking styles by helping you replace the damaging thought with a healthier thought. Click the below link to access Dr. Snooze and then click the cognitive training module to access this feature now at no cost to you!
What Constitutes a Sleep Problem
For more information on whether you think you have a sleep problem, check out Dr. Gartenberg discussing this question in a recent interview.
